People with sleep apnea who can’t tolerate the noise and discomfort of a CPAP machine might benefit from a mouth guard or surgery.
Article Published May 31, 2021
Many people wear a CPAP machine at night to treat the interrupted breathing of obstructive sleep apnea, a condition that affects an estimated 22 million Americans. But CPAP machines can be noisy, cumbersome and uncomfortable, and many people stop using the devices altogether, which can have dire long-term consequences.
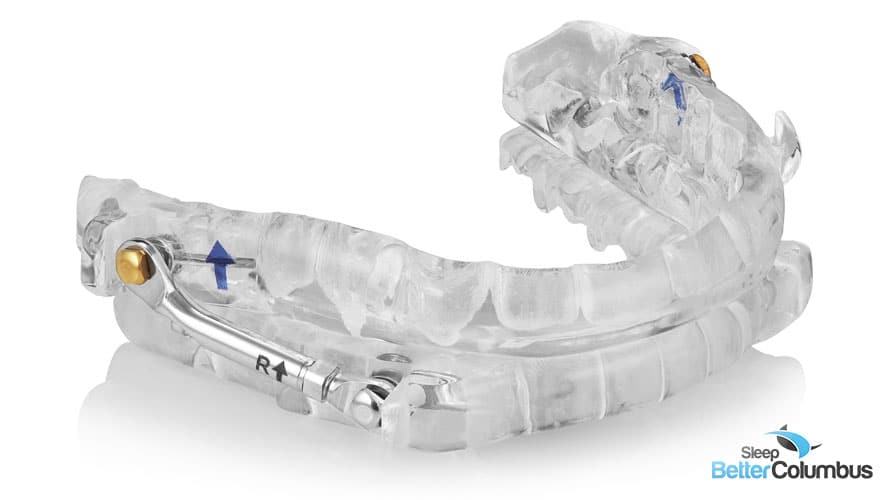
Mouth guards may be a more comfortable and easy-to-use alternative for many people with obstructive sleep apnea, according to a new report. The study, published in Laryngoscope, looked at 347 people with sleep apnea who were fitted with a mouth guard by an otolaryngologist. Two-thirds of patients reported they were comfortable wearing the devices, and the devices appeared to be effective in helping to relieve the disordered breathing of obstructive sleep apnea.
The lead author of the study, Dr. Guillaume Buiret, head of otolaryngology at Valence Hospital in Valence, France, said that if he had sleep apnea, he would choose an oral appliance first.
“It’s easy to tolerate, effective and it costs a lot less than CPAP,” he said. “Thirty to 40 percent of our patients can’t use CPAP, and these patients almost always find the dental appliance helpful. I would recommend it as a first-line treatment”
Loud snoring may be the most obvious consequence of sleep apnea, but the condition, if left untreated, can lead to a broad range of complications, including high blood pressure, heart disease, liver dysfunction and Type 2 diabetes.
The problem develops when the soft tissue at the back of the throat collapses during sleep, blocking the airway. This leads to breathing cessation for brief periods, gasping for air, difficulty staying asleep, and all the problems of daytime sleepiness, from poor job performance to fatal accidents. Animals can have it too — bulldogs, for example, have a narrow airway and a soft palate that can easily block it. Their sleep apnea is almost identical to the human version.
The severity of the condition varies widely from a very mild problem that may need no treatment at all to severe or even life-threatening disease. Dr. Sara E. Benjamin, a neurologist and sleep specialist at Johns Hopkins, said that spending a night in a sleep laboratory monitored by a technician is the best way to diagnose apnea. A lab study offers the most thorough analysis, and can detect many other sleep problems besides apnea, but there are home test kits that are easy to use and cost-effective. They test breathing effort and oxygen levels, but not the brain waves, muscle tone and leg movements that a lab test records.
How can you know that you need a sleep assessment? “It’s a low standard to get evaluated, either by home testing or in a sleep lab,” Dr. Benjamin said. “If a person feels sleep problems are impacting daily activities, that’s enough to go and get evaluated. If the cause is a breathing problem, you don’t want to ignore it.”
A CPAP — continuous positive airway pressure — machine is usually the first option for treating sleep apnea. The device has a motor that delivers pressurized air through a tube attached to a mask that covers the nose, or both the nose and the mouth. This keeps the airway open. Some machines can automatically change the pressure to compensate for changes in sleep position; others require manual adjustment. Headgear varies, but all have adjustable straps to get the right fit. There are newer models that can deliver heated or humidified air, depending on the patient’s preferences, and there are small travel models as well.
“We recommend a custom device made by a dentist,” Dr. Benjamin said. “And you should be retested to see how well it’s working. There’s subjective and objective improvement that should be tracked.”
But there are people for whom neither CPAP nor dental appliances work, either because they cannot use them consistently or correctly, or because the devices themselves do not solve the problem even when used properly. For these patients, there are various effective surgical procedures.
The most common is soft tissue surgery, which involves modifying or excising tissue at the back of the mouth. Depending on the structures and musculature of the mouth, the surgeon can trim the soft palate and the uvula, remove the tonsils, shrink tissues with a heated instrument, straighten a deviated septum, or alter the position of the tongue muscles, all with the aim of improving air flow.

There are also bone surgeries that move the jaw forward to make the entire breathing space larger, a procedure that can involve a protracted recovery period.
In 2014, the Food and Drug Administration approved a device called Inspire Upper Airway Stimulation. This is a small appliance implanted under the skin like a heart pacemaker. Using two electrical leads, it senses the breathing pattern and stimulates the nerve that controls the tongue to move it out of the way and allow air to pass freely. Implanting it is a day surgery procedure that takes about two hours.
“It doesn’t change the anatomy, and recovery is easier than with other surgeries,” said Dr. Maria V. Suurna, an associate professor of otolaryngology at Weill Cornell Medicine who specializes in surgery for sleep apnea. “It’s effective. It has the lowest complication rate of all the surgeries.
“But it’s not for everyone. It’s approved only for adults 18 and older who are not overweight and who have moderate to severe apnea.” Some people may be ineligible because of the structure of their anatomy.
“Surgery is tricky,” Dr. Suurna said. “But there’s no ideal treatment for apnea. Each has pros and cons, benefits and risks.”




